At 37 weeks pregnant with her third child, Alicia Murphy began experiencing contractions that quickly became worrisome as they progressed over just a ten-minute period.
“I had just gotten home from work when my wife told me it was time to go to the hospital. By the time we were ready to go, the contractions had brought her to her knees and her water broke,” says Dr. Lee Murphy, a family medicine physician at Baylor Scott & White in Waco. “I thought we were about to have this baby on our kitchen floor, and I was ill prepared to help her deliver with a pair of oven mitts. Alicia had needed C-sections with both our older children, so I was worried she would need more help than I could provide.”
A short ambulance ride brought them to Baylor Scott & White Medical Center – Hillcrest, where doctors discovered the baby was in distress with a decreased heart rate. Alicia was experiencing placental abruption, a dangerous complication for both mother and baby in which the placenta separates from the uterine wall, often causing the mother to bleed excessively and depriving the baby of oxygen. In addition, the umbilical cord was wrapped around the baby’s neck, a situation that can also reduce oxygen flow.
Doctors and nurses worked to rapidly deliver the baby, helping the parents make a whirlwind of decisions crucial to the health of both infant and mother.
“We were so fortunate to be able to deliver her quickly,” Dr. Murphy says. “The rate of babies who survive placental abruption decreases dramatically after two hours, but it only took a total of 11 minutes from the time we arrived at the ER to the time baby Lynora was delivered.”
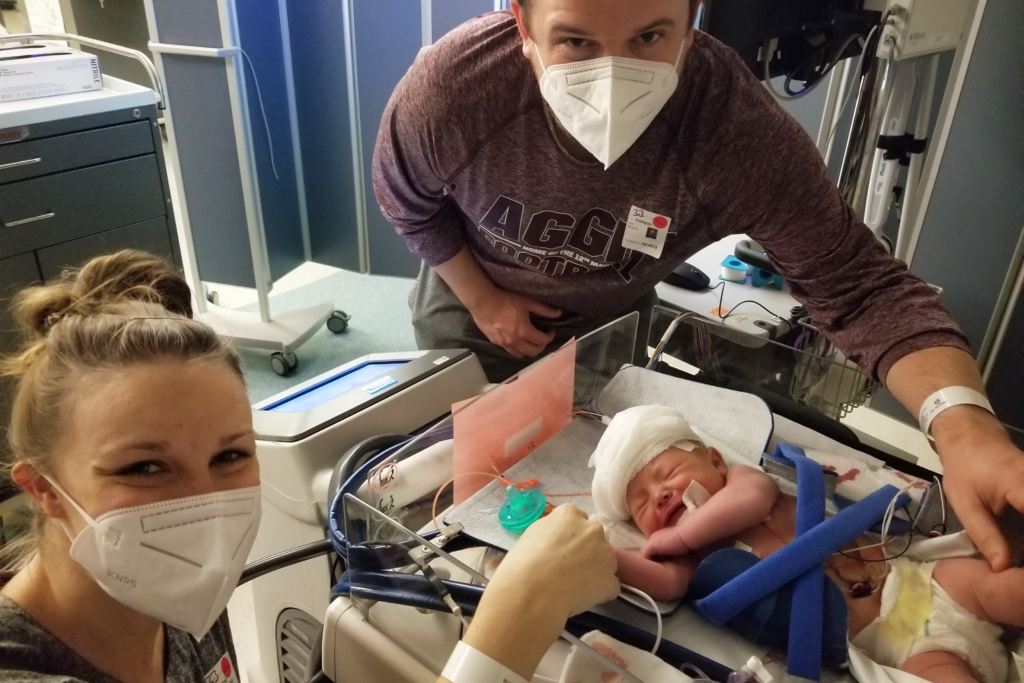
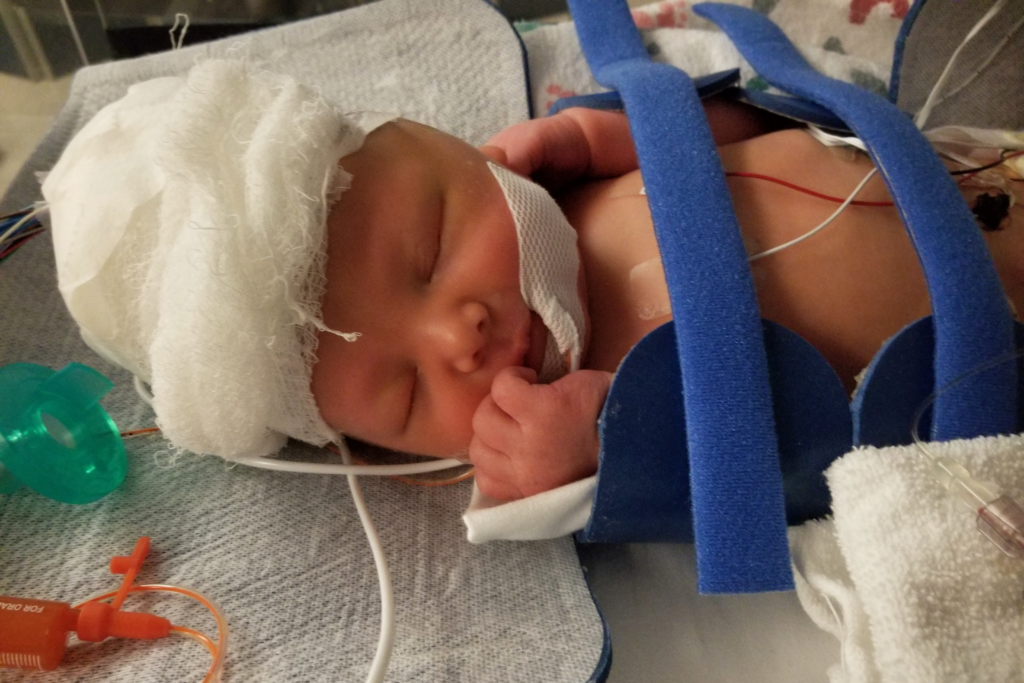

Unfortunately, Lynora wasn’t breathing adequately on her own and needed to be intubated.
“Even as a doctor, it was terrifying,” Dr. Murphy says. “Luckily, she started coming around and was able to have the breathing tube removed within the hour.”
To help mitigate any brain damage caused by the lack of oxygen during her birth, doctors recommended transferring Lynora to the NICU at Baylor Scott & White Medical Center – Temple for 72 hours of cooling therapy.
After her first night on the cooling bed, Lynora’s doctors were cautiously optimistic about her recovery. “After the three days, she began feeding like a champ and was doing all the things you’d expect a newborn to do,” Dr. Murphy says. “When she had an MRI at seven days old, we were so relieved to see that she didn’t have any apparent brain damage.”
Ironically, Dr. Murphy had prior experience with many of the doctors and nurses caring for his daughter. “I worked with one of the nurses who delivered her during my residency in Tyler, and then we ended up in the same NICU where I did a rotation during medical school,” he says. “The doctors and nurses were all so wonderful at explaining everything that was happening and were available for questions at all times. I feel so blessed to work for this organization that has been there for my family.”
Lynora is now about four months old, rolling over, and meeting all the key milestones for infants her age. Her parents and older sisters are over the moon for little “Nory Lou,” as proud dad likes to call her.
“I believe God grants us miracles every day, but He gives us the people and the playbook of modern medicine to help accomplish those miracles,” Dr. Murphy says. “There are so many people who helped deliver Nory into this world—from the doctors and nurses to the donors supplying resources to keep them at the forefront of the latest research and equipment. We plan to make sure she knows all of the miracles that took place in order to bring her into our lives.”